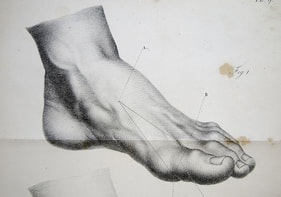
 Problems with pain management are almost always the primary complaint in patients suffering from Ehlers-Danlos Syndrome (EDS). Much of this pain is musculoskeletal in nature such as a sprain, tendinosis or joint subluxation. But often our patient's pain complaints are less clear. This pain can be described as a burning, stabbing pain that moves throughout the body inexplicably and without identifiable causes. Recent research by Cazzato, et al. has demonstrated that patients with EDS have a very high chance of manifesting small fiber neuropathy in the sensory fibers of their skin. Neuropathy is the inflammation or death of nerve fibers in the outer-layers of our bodies. This is commonly seen in diabetic patients with changes in their blood chemistry. However it has recently been identified that more than 90% of investigated EDS patients demonstrate evidence of localized small fiber neuropathy. This has commonly been identified and treated in the fibromyalgia populations with medications such as Neurontin/Gabapentin, Amitriptyline, Pregabalin and Cymbalta. This type of pain would be classified as neuropathic pain and is very different from mechanical type musculoskeletal pain. Pain medications like NSAID, opioids and muscle relaxants that are prescribed for musculoskeletal pain are often unsuccessful for treating neuropathically induced pains. The Cazzato study reported 19 of 24 EDS patients complained of moderate to severe symptoms consistent with neuropathic pain. When their research patients were examined via skin biopsy all 24 demonstrated findings consistent with small fiber neuropathy. When discussing pain medication with your providers it is important to identify what the underlying pain generators are in order to pick efficacious medicines and interventions. If your pain is a diffuse burning discomfort that bounces around the surface levels of skin, fascia and muscle you may benefit from a medication specifically targeting neurogenic pain. Not sure where you pain is coming from or why? That is a great reason to come see a Physical Therapist who can manually test your body and evaluate your symptoms to provide direction and advice about the best course of action. As a Doctor of Physical Therapy with advanced training it would be my pleasure to evaluate and assess what is going on to help you find relief and develop a plan of action that will lead to better quality of life. Email me or call 360-952-3074 to request an appointment today for more information. ~Brian Kitzerow, DPT, CMPT, OCS
 www.runwaypilates.com www.runwaypilates.com We all know that there are several benefits that occur from participating in regular exercise. But is exercise specifically helpful for the hypermobile type Ehlers Danlos Syndrome (hEDS) population? And if so, how and why? We have good evidence that exercise is helpful for many components of our lives. It helps with hormonal control of estrogen, testosterone, progesterone and cortisol. It improves sleep cycles and the hormones involved in regulating our sleep patterns. It helps improve muscle mass and prevents the loss of bone density. Exercise participation is strongly correlated with reductions in stress, anxiety, and depression, and improvements in mood and the sense of well-being. Exercise is linked with improvements in coordination and decreases in fall risk. Improvements in cognition, focus, and memory are also linked with exercise participation. There has been strong evidence demonstrating that unstable joints are improved with exercise and that exercise can reduce daily pain levels. As you may or may not know, EDS is a connective tissue disorder. As connective tissue is widespread throughout the body, EDS has wide-ranging effects. Joints are less stable and have a higher incidence of injury and subluxation. Balance (or proprioception) is reduced raising the incidence of falls. Bone density can be effected. Muscle strength is commonly lower in this population (which some researchers have connected with joint proprioception deficits and others with fear of movement). Dysfunctional movement patterns are adopted with impaired coordination. And many different types of pains are experienced. But is exercise beneficial for patients with joint hypermobility syndrome (JHS) and hEDS? Research is suggesting yes for many reasons. Kemp looked at young patients over a six-week exercise course in one of two groups. One group had a generalized strength and conditioning program, and the other group had a more focused joint stabilization exercise program. Both groups demonstrated decreases in pain levels and functional assessment (roughly 30% improvement!) but the focused group also demonstrated more parental perceived functional gains. Studies by Sahin, Pacey, and Celenay all found similar responses with improvements in both function and comfort. A systematic review (assessment of all the available literature that the authors can find) in 2014 also found evidence for the use of balance retraining based exercises. There is also limited evidence that just like hEDS, classical EDS (cEDS) responds well to exercise. Moller looked at three cEDS patients who were treated with “heavy” strength training 3 days per week. Measurements of the patellar tendon demonstrated improved strength of the tendon connective tissues from 1795 N/mm to 2519N/mm (>70% increase in strength). Energy levels and perceived strength were both improved in all subjects. And even though these exercise routines were very intensive, pain levels did not increase at the end of the study for 2 of the 3 subjects and were actually lower in the third subject. In conclusion, the research is currently very supportive of exercise to improve function and comfort in the hEDS, JHS, and cEDS populations. It appears that there are better results from emphasizing trunk stabilization and balance based exercises, but all types of exercise studied showed improvements. It can be very helpful to be treated under the supervision of a physical therapist to oversee a controlled, graded progression of your program, as well as to address existing injuries with manual interventions as they interfere with your exercise program. Clinical experience suggests that exercise is the key intervention to return freedom, function and comfort in your life. Though connective tissue may be lax, muscle remains responsive to exercise and strength needs to be emphasized to compensate for ligamentous laxity. Do or someone you know suffer from EDS? Do you suspect but are unsure? Considering coming to All Ways Well for an assessment from an experienced Physical Therapist. Email me questions or request an appointment online today. ~Brian Kitzerow, DPT
 Summer is upon us and the rainy weather seems long gone! Or at least dormant. With more good weather many of us will be subtly tempted to increase our training intensities and want to stay out for that extra mileage. Though it is a good idea to increase our strength and endurance, doing so in a thoughtless manner often leads to injuries that can set our training back a month or more. Proximal hamstring tears, achilles tendinosis, calf lesions, plantar fasciosis, stress fractures, low back pain and patellar femoral syndrome (PFS) are all common running injuries that are more likely to occur when training regiments are progressed too quickly or when tissue damage is happening too consistently for the body to have an opportunity to strengthen the stressed tissues. Irintchev studied muscle damage in mice and concluded that “acute muscle injury occurring upon onset of voluntary running is a usual event in the adaption of muscles to altered use”. Additionally, muscle damage appears to have to occur in order to progress strength levels. We know that muscle is very plastic and thoroughly regenerative. It is one of our body’s most repairable tissues. The problems arise when the quantity and frequency of healthy injury begins to exceed the body’s ability to repair it. So how do we balance the natural damage we do to our body, with our body's ability to handle it while progressing a running program? One long-time guideline has been the 10% rule. Meaning we don’t progress our running distance greater than 10% in one week. The main problem with this rule is its’ over-simplification, but that is also one of its’ main strengths. This rule gives you a basic guideline and doesn’t require a great deal of analysis and oversight to ensure that your response to the increased workload isn’t approaching an unhealthy level. You can pad the 10% rule for a greater probability of success by monitoring your response to exercise. Muscle pain tends to be healthy, but pain at your tendons, especially where they interface with their bony attachments tends to indicate overuse. Additionally, pain in the bones of your feet or around the joints of your hips and knees also can show excessive inflammatory responses that may precede more serious injury. Recovery is essential. Inflammatory processes typically peak after 48 hours suggesting that taking an extra day of recovery if you start to suspect early injury may be very helpful for extending injury-free long-term training. Though consistency is important for form and coordination, changing the stresses on your body can help you train harder and longer. Consider alternating your running shoes between two similar styles or brands to change the distribution of forces through your lower extremities. Work in progression style runs where your pace increases at different points from beginning to end of your run. Or work in other forms of aerobic and resistive exercise. As you increase your runs this year do it safely and with good awareness of your strategies and physical responses to raise the odds of success. By Brian Kitzerow, DPT, OCS, CMPT Lee A, Anderson J, Joya J, Head S, Pather N, Kee A, Gunning P, Hardeman E. Aged skeletal muscle retains the ability to fully regenerate functional architecture. BioArchitecture. 2013;3(2):25-37 Irintchev A, Wernig A. Muscle damage and repair in voluntarily running mice: strain and muscle differences. Cell and Tissue Research. 1987;249:509-521 Buford T, MacNeil R, Clough L, Dirain M, Sandesara B, Pahor M, Manini T, Leeuwenburgh C. Active muscle regeneration following eccentric contraction-induced injury is similar between healthy young and older adults. Journal of Applied Physiology. 2014;116(11): 1481-1490.  Pain is a multifaceted and deeply personal experience that can be very difficult to describe and communicate. Pain itself is a very functional experience that warns us to be careful when we might be injuring ourselves. We can see how important pain is in the rare occurrences in which a person is born without the capacity to experience it. This condition is known as congenital analgesia and these individuals have a very high mortality rate as they struggle with repeated broken bones and poor healing rates due to tissue re-injury when they can’t feel that they are hurting themselves. It is important to consciously acknowledge that pain is a functional sensation and that when properly manifested and interpreted can be very beneficial to our health and self-care. Especially when we know what the pain signals we experience mean. When it becomes too prolific, though, it can be impossible to negotiate recovery on your own. Most people are very good at pushing through their symptoms so that they can be functional throughout the day. Unfortunately, they commonly do this by categorizing unpleasant pain impulses into a single amorphous uniculture they relate to as “my pain”. Everything from a skinned elbow to headache to stomach cramping gets thrown into the same classification schema with little thought about what each individual signal might mean. Though this can be very useful in the short-term, this strategy tends to inhibit long-term recovery because they get re-injured over and over. Just like in the congenital analgesia population, utilizing this strategy to ignore pain tends to worsen symptoms and pain levels over time because it doesn’t allow healing. Unaddressed injuries start to pile up on top of each other and it gets very hard to determine what the pain you are feeling means. This is similar to driving your car with a flat tire; you will make it a little further and might even make it home, but you will have destroyed your wheel, axel and engine by the time you do. If you don’t address the underlying problem (your tire is flat) you can’t take care of the other problems (your speed has slowed down, the ride is bumpy and there is a horrible smell from your car starting to burn). The original centrally driven model of pain is usually attributed to Descartes and was a simple circuit-like reaction where pain was stimulated at the site of injury and went directly to the brain with no control for grading or interpretation. We now know that this is inaccurate. Pain is an experience that our brains create. This was detailed in the neuromatrix theory described by Ronald Melzack in the 1960s and expanded upon by many highly insightful researchers like Lorimer Mosely and David Butler. Our brains absorb all the thousands of input signals coming in to them at one time; the sensation of that needle poking our arm, the comforting smells of cookies baking, the angry, stern looks of our employer speaking to us, the full, satiated feeling in our stomach, the sound of breaking glass. After that the brain filters these inputs through our previous learned experiences (the last time I saw a heavy hammer falling it landed on my foot or I was brutally spanked after I heard that crashing sound as a child and I broke the dishes). It then decides what it should bring from the unconscious experience into our conscious awareness. If the brain decides that the input isn’t relevant to our survival it won’t tell us about the pain stimuli. We commonly see this in imaging studies where 60-70% of the healthy population have a hip or spine injury that they are not impacted by or aware of it in the slightest. Sometimes the brain and sensory neurons become over-responsive at interpreting inputs as pain. What was previously benign and safe (like light touch or a gentle walk) can become very painful. Even when there isn’t any tissue damage. This is termed a Central Pain Processing Dysfunction and recovery requires treatment to desensitize the central nervous system and remind it of what good and bad stimuli should feel like when determining whether you should hurt or not. There has been a swing in pain medicine to treating centrally driven pain with a technique that some psychologists utilize to treat fear and anxiety known as Acceptance and Commitment Theory (ACT). This approach emphasizes focusing on goals and accepting that pain is an inevitable consequence to reaching them. For instance, I know that walking two miles is going to make my back hurt worse afterwards, but I enjoy walking and need to get to the store. So I am going to accept that I will be pushing myself beyond what my body is telling me it is capable of and commit to walking anyway (or you could have been more insightful to what your body was saying and walked one mile, rested and then finished with no increase in pain and a progressively stronger body). This approach however ignores that at the root of central pain processing dysfunctions, are usually initial and subsequent injuries that stimulated the brain to become hypervigilant in the first place. This is particularly true in the Ehlers-Danlos Syndrome (EDS) population who always have underlying musculoskeletal dysfunction contributing if there is a central pain processing dysfunction. ACT based treatments for addressing pain are similar to driving home with that flat tire. Sure, you can accept that your tire is flat and that you are damaging your car driving it home instead of addressing the flat tire, but your car isn’t going to benefit from it. In the same way your body won’t benefit from ignoring your pain instead of analyzing what the pain means. Cognitive Behavior Theory (CBT) is a psychological technique that works very well with pain medicine and particularly well with the EDS population. This theory suggests that you cognitively assess and investigate what you are feeling. You then decide on an action based on the logical conclusions you make from what the pain is trying to communicate to you. Very often when we cognitively assess our pain we can tell that this is a very short term and temporary complaint that probably won’t be there tomorrow, such as a sharp, brief stab in the shoulder or a sore thigh muscle. These are things that we can consciously let go of as they are not serious and are unlikely to affect us long-term. In effect, we are performing on a conscious level the duties that our unconscious pain processing centers should be performing unconsciously. This has very strong benefits to reducing stress and anxiety because we know these pain experiences will be temporary and are not threatening to our wellbeing. Other times, when we utilize CBT, we recognize that a pain is either more severe, or has been a consistent problem that might indicate damage to our tissue in some way. In this case we are in a position to cognitively assess what kind of pain we are feeling and what that might indicate. Is this a tendon pain that indicates we aren’t stabilizing our shoulder with our scapular muscles and our rotator cuff is irritated? Do we see less pain (and by default less tissue damage) when we lift a little less? Or engage our low traps before lifting the arm? When our rotator cuff is more active and strong, is this pain consistently less? Or instead of the shoulder is this a burning, nervy pain around our skin and fascia that indicates small fiber neuropathy (as seen in fibromyalgia and very strongly in the recent EDS research)? In that case we could benefit from talking to our doctors about a neurogenic pain medication and lowering our baseline inflammation levels. Is this the headache that starts at the back of our skull and rolls over the skull to sit behind our eyes? In that case we are probably scrunching the circulation of our greater occipital nerve and need to relax our neck muscles and change our posture, or strengthen our core and shoulder muscles to improve our ergonomics. CBT-based approaches gives back to you the control to manage your symptoms instead of being placed in the position of a passive victim. There will be some pains that are unresponsive or have so much complicated noise going on that you will need a good PT, MD or body worker to help with them, but commonly you can have a lot of control over your daily experiences. It is just important to know what the different “flavors” of pain signals suggest. Be cognitively aware and assess your symptoms as they come up. Some will be transitory and unimportant. Others will be more important to listen to and adjust the intensity of how you’re moving and working at in order to allow your body to heal. Your physical therapist can help you negotiate what different pains mean and how to manage them successfully. Brian Kitzerow is a Doctor of Physical Therapy at Good Health Physical Therapy with offices in both SW and NE Portland. Interested in learning more about your own pain? Consider seeing Brian at Good Health or coming in for Acupuncture at All Ways Well today!  According to a recent article in the Journal of Orthopedic and Sports Physical Therapy Anterior Cruciate Ligament, or ACL, rupture is “one of the most physically, financially, and emotionally devastating sport-related knee injuries,” which is something I can personally attest to. I tore my ACL in 2003 and had reconstructive surgery because I wanted to return to sport which, at the time, was martial arts. I had good insurance then as well so my out of pocket costs were manageable, but I remember seeing the hospital bill - $50,000. It took an entire year of weekly acupuncture and Physical Therapy for me to participate in my sport at the level I wanted to, and it was two years before I didn’t notice my knee feeling different during activity. I am proud to say, however, that one year after my surgery I successfully completed a very vigorous 24 hour martial arts test including 12 hours of continuous fighting, running and forms. A decade later, my ACL repair is still holding strong with no concerns. What I didn’t know until I read this article, was how rare my case is. Only 44% of athletes successfully return to sport after an average 3-1/2 years following an ACL repair. When quizzed about their subjective experience of performance after a successful ACL repair and return to sport, only 50% percent of high-school and college athletes indicated that they were able to perform at their pre-injury level. Furthermore, up to 30% of athletes who return to sport after an ACL repair re-injure their ACL or tear the ACL on the opposite knee due to a number of factors, neuromuscular weakness and asymmetry primary among them. Due in part to the increased joint laxity and increased angle between hip and knee, female athletes with previous ACL repair are 4 times more likely to re-injure their knees after returning to sport compared to their male counterparts! My ACL repair actually puts me in the top 5% of female athletes who have an ACL repair. I absolutely credit my success to the individualized and dynamic Physical Therapy I received along with consistent Acupuncture treatments. I actually started acupuncture two days after my surgery and continued treatment every week for an entire year, and then every other week for 2 years thereafter. Even my surgeon was amazed with my recovery (and he was the surgeon for the Blazers here in Portland). Preventing an ACL InjurySo if you are engaged in sport, how do you prevent an ACL injury? Sometimes you just can’t, life happens, but you can greatly decrease the possibility of injury with proper neuromuscular training. According to this research article, of primary importance are the following:
Regular acupuncture is also recommended. Acupuncture can decrease and resolve minor aches and pains, keep muscles physically loose and energetically balanced, and cause natural endorphins and anti-inflammatories to be released by the body improving performance and recovery rates for minor injuries. Recovering from an ACL InjuryIf you are unfortunate enough to experience an ACL injury or tear, there is still a lot you to can do to ensure a strong recovery and decrease your likelihood of experiencing a secondary ACL injury.
My go to Physical Therapist for knee injury prevention, knee injury, ACL injury and ACL surgery recovery is my husband - Brian Kitzerow, DPT at Goodell Physical Therapy. He always keeps up on the latest research and has a thoughtful and thorough approach to every patient.  According to the Oregon Department of Transportation there were 49,798 car accidents reported in 2012 and 36,085 people were injured in those accidents. That is an average of 136 crashes PER DAY in Oregon alone! And did you know that the highest incidents of crashes occurred on Fridays and in October? [Note to self; try not to drive on Fridays in October!] All levity aside, a car accident is no joke, as the 36,000 injured people in 2012 can attest. The force of impact that the body is made to endure in even a minor car accident causes a ripple effect of muscular tension which can result in whiplash, headache, back pain, decreased range of motion and sciatica to name just a few. None of these things should be left untreated and the sooner you get in for treatment, the sooner you can head off pain and injury in the early stages and avoid major problems down the line. Some of these effects such as whiplash are immediate, but others occur due to compensation over time and the best remedy is to get treatment early - within the first two weeks of an accident ideally. Acupuncture for auto accident recovery is highly effective, and if you combine acupuncture with Physical Therapy and Massage your recovery is expedited even more. Acupuncture by itself gives great hope for recovery. It can:
Testimonial from an Auto Accident Treatment PatientAfter my auto accident, my pain levels made it hard for me to both concentrate and to physically sit long enough to do my work. My acupuncture treatments with Rebecca were and continue to be a critical part of my recovery from the accident, as they provided immediate relief for the acute pain and gave me three or four days of respite from it after treatment. Of all the healing modalities I tried - massage therapy, chiropractic treatment, physical therapy, and acupuncture - acupuncture proved to be the one that was the best at keeping pain to manageable levels, thus allowing me to get back to the work I love doing. Combining Modalities in Car Accident Treatment Gives Best ResultsMassage or foot reflexology is something I add into all of my acupuncture treatments for at least 5-10 minutes, but I encourage all patients who come in for auto accident treatment to come in for 90 minute acupuncture + massage sessions so we have more time to spend on bodywork (massage). It helps that if you have an auto accident in Oregon, acupuncture and massage are covered 100% by your auto insurance without a referral!
I often incorporate Cupping and Gua Sha - traditional Chinese myofascial release techniques to relieve pain and stagnation - into car accident treatments as well. This too, I find, helps patients recover faster after an auto accident or MVA (motor vehicle accident) by helping the body relieve tension and flush out toxins that may be associated with tense guarded muscles. Lastly I always recommend patients see a Physical Therapist as part of their car accident treatment plan, because while acupuncture can help balance the body, reduce and often completely relieve pain from whiplash, headache, back spasm, sciatica and certainly helps to increase range of motion, it can’t assess your posture or potential repetitive motion injury sources in your daily life that could aggravate your pain and delay healing. In my experience as both a motor vehicle accident treatment patient AND a provider, no one is a better mechanic for the body than a Physical Therapist, and when you combine the pain relief and Qi balancing of Acupuncture and massage, with the mechanical reprogramming of physical therapy exercise, your results are quick and long lasting. The most important message here is that no matter what you do, get treatment early. Ideally within those first two weeks of having a car accident. Sometimes it takes 10-14 days for the full effects of a car accident to “wear in” to the body, so if you can get in before your body really sets into the pain, you have a much better chance of heading it off and avoiding the worst effects the injury has to offer. If you have questions please don’t hesitate to contact me via email or book a free consultation anytime. If you’ve had a car accident and are looking for treatment, please book in for a new patient 90 minute appointment so we can assess your situation and we will take it from there! I have excellent Physical Therapists in SW, SE and downtown that I refer to for auto accidents regularly and I would be honored to help coordinate your care. Until next time, ~Rebecca I am very excited to announce that my husband, Brian Kitzerow, DPT, is now working at Goodell PT in SW Portland and is accepting new patients! We are very excited that he is working in an outpatient setting and that we can share referrals now. I was so excited that I had to blog about it, and I can't wait to see what our collaborations bring for our patients. With a strong background in biochemistry, a long history of physical activity including soccer, track & field and martial arts, he has the education and experience to excel in his work and I can tell you that he does. He has a special interest in chronic and neuropathic pain and is enjoying working with ESD patients in particular - a specialty at Goodell. ESD stands for Ehlers-Danlos Syndrome, an inherited connective tissue disorder, so if you know anyone with chronic pain, EDS, neuropathic pain or someone who has been in a car accident lately, please think of sending them his way with Rebecca's double thumbs up.
I also have to share that I believe the combination of Acupuncture and Physical Therapy can be pretty amazing. It can be difficult to commit to so much regular treatment, I understand that (from experience), but if you can commit to the time required to combine therapies, your results will be accelerated and longer lasting.
Acupuncture can straighten out your energetic system, decrease stress and pain, and re-habituate your body to a state of balance. Physical Therapy will balance the body physically, improve strength and flexibility, and give you the tools you need to heal and continue your preferred activity level without incurring new injury. Its a winning combination because the two approaches are just the right amount of different and complementary. I feel like a personal testament to this powerful combination because while you may not think it to look at me, I've had a lot of injury in my life. I've had tendonitis, bursitis, meniscus frays and tears, ACL tear and knee surgery, piriformis syndrome, dislocations, subluxations, back spasms and a motor vehicle accident. I'm one of those people that dreads filling out new medical forms because there is never enough room for all my injuries on there and because the doctor usually gawks at my list. This long list, however, means I am very well acquainted with pain and pain treatments experientially and professionally, and I have no problem sharing that my best results have come from combining Acupuncture and Physical Therapy. That is why I am so excited to be able to refer patients to my husband in this setting because I know he is top notch and an excellent physical diagnostician. That is also why I often recommend Physical Therapy - its effective, covered by insurance, and gives YOU tools that you can take home with you and apply to the way you use your body for years to come. So with this note, please welcome my husband to the world of outpatient clinics, and if you have a physical therapy need or know someone who does think about sending them his way! Until next time, ~Rebecca |
AuthorsRebecca M H Kitzerow is a Licensed Acupuncturist practicing in La Center, Washington. With over a decade of experience she has won 10 Nattie consumer choice awards from Natural Awakenings Magazine since 2014. Archives
July 2024
Categories
All
|
Photos from Hey Paul Studios, BeGreen_Studio, Pawel Pacholec, 1950sUnlimited, toulupaliaqaz, Joelk75, OnTask, Robert Gourley, cnu_sports, Mitya Ku, wuestenigel (CC BY 2.0), FootMassagez, 401(K) 2013, Mariana Heinz, @EdwardTerry, fishhawk, liverpoolhls, torbakhopper, Boemski, dolomitibl, Driscolltheque, Dave n Laura, Vaping360, MVWorks, Life Mental Health, MVWorks, mikefats, Scot Nelson, jfl1066, wZa HK, ruurmo, Guadalupe Cervilla, Army Medicine, GViciano, torbakhopper, adrigu, Saulo Cruz, Ben Cumming, marniejoyce, kcxd, JasonCorey, kanenas.net, Live to Create Photography, gm.esthermax, Unique Hotels Group, Zenspa1, mysiana, Tobias Lindman, Leader Nancy Pelosi, Kristoffer Trolle, swanksalot, Bill Selak, Parker Knight, stimpsonjake, Gedankensprudler, SuperFantastic, tonynetone, marniejoyce, JeepersMedia, Illusive Photography, 'Ajnagraphy', Iban Torras, scotted400, gtall1, dvanzuijlekom, BPPrice, Skley, torbakhopper, Renato Ganoza, anka.albrecht, QUOI Media, Public Domain Photos, Instant Vantage, Victor Tongdee, Free Grunge Textures - www.freestock.ca, sportEX journals, Nadja Tatar, angela n., marniejoyce, MVWorks, Karolina Kabat, Thomas Fisher Rare Book Library, UofT, ginnerobot, tracilawson, haven't the slightest, My Photo Journeys, Pierre Willemin, Florena_Presse, SuperFantastic, colindunn, zzkt, TraumaAndDissociation, ER24 EMS (Pty) Ltd., shixart1985 (CC BY 2.0), marniejoyce, Tomás Fano, freestock.ca ♡ dare to share beauty, Archives New Zealand, Jaykhuang, airdrie.m, Go-tea 郭天, OnTask, wuestenigel, focusonmore.com, Disney | ABC Television Group, Andrew Gustar, Didriks, ConstructionDealMkting, charlywkarl, barnimages.com, Lel4nd, runwaypilates, michaelstephanfotografie, McLevn, TraumaAndDissociation, eLife - the journal, Lars Plougmann, wuestenigel, shixart1985, boviate, davis.steve32, kevin dooley, @the.photoguy (insta), frederic.gombert, Feathering the Nest, Victor Tondee, shixart1985, wuestenigel, Joe K Gage, kennethkonica
 RSS Feed
RSS Feed
